May is Mental Health Awareness Month, a time to shine a light on the deep connection between mental health and substance use. If you’re struggling with both depression and drinking, anxiety and drug use, or PTSD and addiction, you’re not facing two separate problems. You’re dealing with what’s called a dual diagnosis or co-occurring disorders, and you’re far from alone.
According to the Substance Abuse and Mental Health Services Administration (SAMHSA), nearly 9.5 million adults in the United States experience both a mental health disorder and a substance use disorder in the same year. Yet less than half receive treatment for either condition, and even fewer get the integrated care they need for both.
Here’s what many people don’t realize: treating mental health and addiction separately rarely works. One condition feeds the other in a cycle that keeps you stuck. But when both are addressed together through integrated dual diagnosis treatment, recovery becomes not only possible; it becomes powerful.
In this guide, you’ll learn what dual diagnosis really means, why these conditions so often occur together, and what evidence-based treatment approaches actually work when you’re facing both challenges at once.
If you’re ready to take the first step, Heartfelt Recovery Centers offers personalized dual diagnosis treatment in Hudson, New Hampshire. Call us today at (603) 207-1633 for a confidential assessment.
What Is Dual Diagnosis? Understanding Co-Occurring Disorders
A dual diagnosis means you’re experiencing both a mental health condition and a substance use disorder at the same time. These are also called co-occurring disorders because they happen together, influence each other, and need to be treated as connected rather than separate issues.
Common combinations include:
- Depression and alcohol use disorder
- Anxiety disorders and prescription drug dependence
- Post-traumatic stress disorder (PTSD) and substance use
- Bipolar disorder and drug or alcohol addiction
- Attention-deficit/hyperactivity disorder (ADHD) and stimulant use
The relationship between mental health and addiction isn’t simple. Sometimes mental health symptoms lead people to use substances as a way to cope. Other times, substance use triggers or worsens mental health problems. Often, both conditions develop from shared risk factors like trauma, genetics, or chronic stress.
What’s most important to understand is this: having a dual diagnosis doesn’t mean you’re broken or beyond help. It means you need a treatment approach that addresses the whole picture (your mental health, your substance use, and how the two interact in your life).
At Heartfelt Recovery Centers, our dual diagnosis specialists understand these complex connections. We don’t treat your addiction in isolation or your mental health as an afterthought. Our personalized care plans address both conditions simultaneously, using evidence-based therapies proven to help people heal and build lasting recovery.
Why Mental Health and Substance Use Often Occur Together
Understanding why mental health disorders and substance use so often happen together can help you make sense of your own experience and realize you haven’t done anything wrong.
Self-Medication: Using Substances to Cope
One of the most common reasons people develop co-occurring disorders is self-medication. If you’ve been struggling with untreated depression, anxiety, or trauma, substances might have initially seemed like a solution.
Alcohol can temporarily quiet anxious thoughts. Opioids can numb emotional pain. Stimulants can provide energy when depression makes everything feel heavy and impossible. The problem is that these effects are short-lived, and over time, your body and brain adapt. You need more of the substance to feel the same relief, and when the effects wear off, your mental health symptoms often come back worse than before.
You weren’t trying to develop an addiction. You were trying to survive difficult emotions and experiences. But self-medication creates a trap where the substance becomes part of the problem rather than the solution.
How Substances Affect Mental Health
Even if your substance use started for other reasons, alcohol and drugs directly impact brain chemistry in ways that can trigger or worsen mental health conditions.
Alcohol is a depressant. While it might help you relax initially, chronic drinking disrupts neurotransmitters like serotonin and dopamine (the same chemicals involved in regulating mood). Many people develop symptoms of depression or anxiety as a direct result of prolonged alcohol use.
Stimulants like cocaine or methamphetamine flood the brain with dopamine, creating intense highs followed by crashes that can trigger anxiety, paranoia, and depression. Marijuana, often seen as harmless, can increase anxiety and trigger symptoms in people predisposed to certain mental health conditions.
Opioids interfere with the brain’s natural endorphin system, making it harder for your body to regulate pain and pleasure on its own. When you stop using, both physical and emotional pain can feel overwhelming.
The bottom line is that substances change your brain in ways that make mental health struggles worse, which is why treating both together is essential.
The Vicious Cycle of Co-Occurring Disorders
Once both conditions are present, they create a reinforcing cycle that’s hard to break:
You feel depressed, so you drink to feel better. The alcohol provides temporary relief, but it worsens your depression over time. Your worsening depression leads you to drink more. The drinking causes problems in your life (relationship conflicts, work issues, health concerns). These problems add more stress and worsen your mental health. So you drink even more to cope.
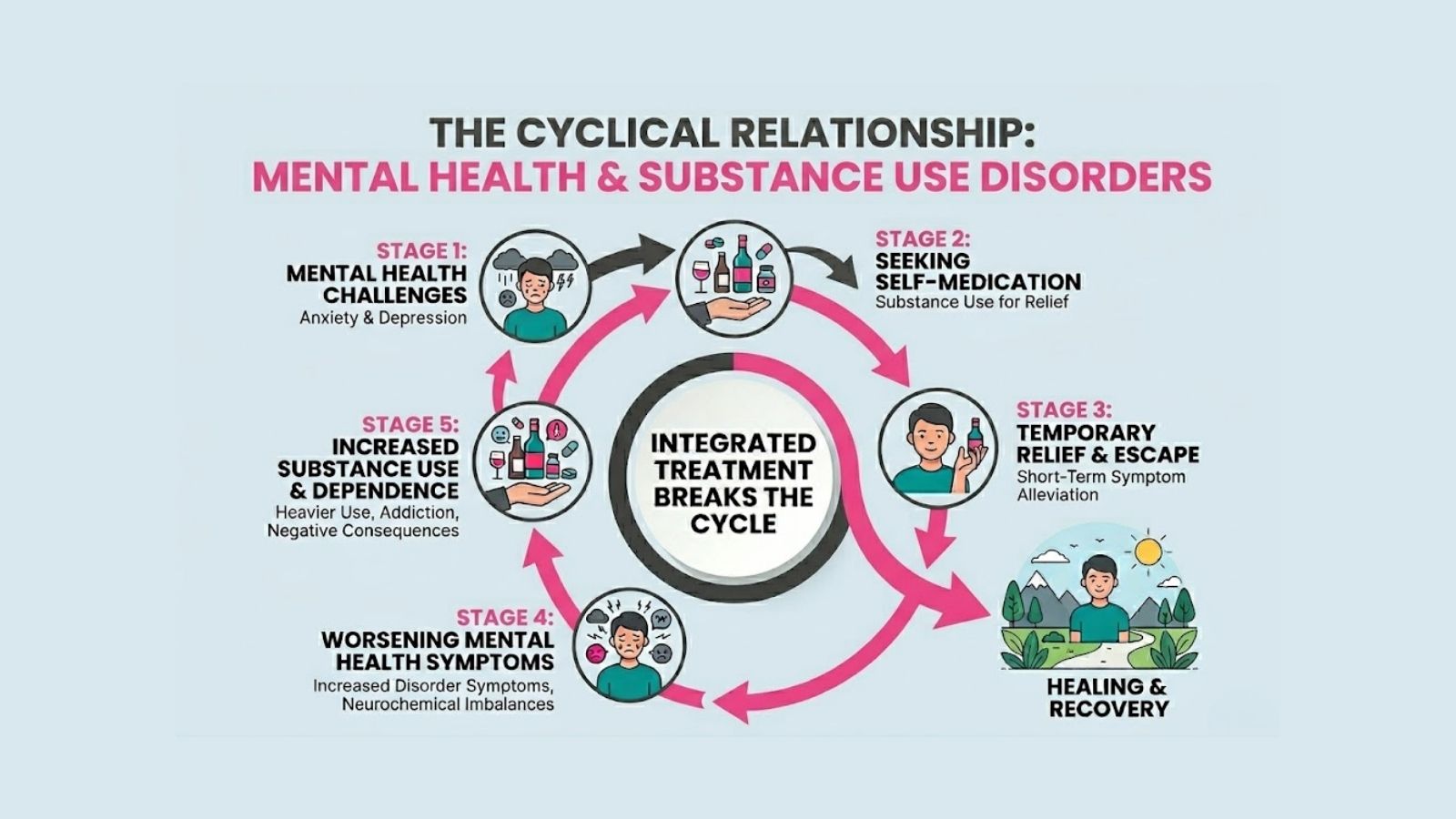
This cycle can feel impossible to escape without help. Traditional treatment that only addresses your substance use might help you stop drinking or using drugs temporarily, but if your underlying depression, anxiety, or PTSD isn’t treated, you’re left struggling with the same unbearable feelings that led to substance use in the first place. Relapse becomes almost inevitable.
That’s why integrated dual diagnosis treatment is so critical. When both conditions are addressed simultaneously, you learn healthy coping skills, receive appropriate medication if needed, and begin healing from the underlying issues driving your substance use.
Common Mental Health Conditions That Co-Occur with Addiction
Dual diagnosis can involve many different combinations of conditions. Here are some of the most common mental health disorders that co-occur with substance use:
Depression and Substance Use Disorder
Major depressive disorder is one of the most frequently diagnosed mental health conditions among people with substance use disorders. The relationship goes both ways: people with depression are more likely to develop addiction, and people with addiction are more likely to develop depression.
Signs you might be experiencing both include persistent feelings of sadness or emptiness, loss of interest in activities you used to enjoy, changes in sleep or appetite, feelings of worthlessness, and using alcohol or drugs to numb emotional pain or fill the void.
Treatment for co-occurring depression and addiction involves addressing both the substance use and the underlying mood disorder through therapy (especially Cognitive Behavioral Therapy), possible antidepressant medication, and lifestyle changes that support both mental health and recovery.
Anxiety Disorders and Addiction
Anxiety disorders (including generalized anxiety disorder, panic disorder, and social anxiety) are extremely common among people struggling with substance use. You might drink to calm your nerves before social situations, use benzodiazepines to manage panic attacks, or turn to marijuana to quiet racing thoughts.
The problem is that while substances might provide short-term relief, they ultimately make anxiety worse. Alcohol withdrawal can trigger panic attacks. Stimulants can increase anxiety symptoms. Even marijuana, which many people use for anxiety, can lead to increased anxiety over time and during withdrawal.
Effective treatment combines evidence-based therapies like Cognitive Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT) with healthy coping mechanisms for managing anxiety without substances.
PTSD and Substance Use
Post-traumatic stress disorder and addiction are deeply connected. Research shows that up to 75% of people who’ve experienced severe trauma also develop substance use issues. Trauma survivors often use substances to manage flashbacks, nightmares, hypervigilance, and the emotional pain that comes with PTSD.
Treating co-occurring PTSD and addiction requires specialized trauma-informed care. This means working with therapists who understand how trauma affects the brain and body and who use approaches specifically designed to process traumatic memories safely, such as Eye Movement Desensitization and Reprocessing (EMDR) or trauma-focused CBT.
At Heartfelt Recovery Centers, our trauma-informed approach recognizes that your substance use may be connected to experiences you’ve survived. We create a safe, supportive environment where healing from both trauma and addiction can happen together.
Bipolar Disorder and Addiction
Bipolar disorder involves extreme mood swings between manic or hypomanic episodes (high energy, racing thoughts, and impulsive behavior) and depressive episodes (low energy, sadness, and hopelessness). Substance use is extremely common among people with bipolar disorder, with studies showing that up to 60% will struggle with addiction at some point.
During manic phases, increased impulsivity and poor judgment can lead to heavy substance use. During depressive phases, you might use substances to cope with overwhelming sadness. Substances can also trigger mood episodes or make them more severe and harder to manage.
Treatment for co-occurring bipolar disorder and addiction requires careful medication management (mood stabilizers are essential for bipolar disorder) combined with therapy, routine establishment, and close monitoring by psychiatric professionals.
Why Traditional Addiction Treatment Falls Short for Dual Diagnosis
If you’ve been to treatment before and it didn’t work, or if you’re researching options and feeling overwhelmed, you need to understand why traditional, single-focus addiction treatment often fails people with co-occurring disorders.
The problem with treating one condition at a time is that you’re only addressing half of what’s keeping you stuck. If you go to addiction treatment that doesn’t address your depression, you might successfully detox and learn relapse prevention skills, but you’re still left dealing with the crushing weight of depression that made you turn to substances in the first place. Without tools to manage your mental health, relapse is almost inevitable.
On the flip side, if you see a therapist for depression but they don’t address your substance use, therapy might help you understand your emotions better, but the substances you’re using are actively working against your mental health recovery. You can’t effectively treat depression while alcohol or drugs are sabotaging your brain chemistry.
Sequential treatment doesn’t work either. Some programs try to treat addiction first, then address mental health afterward (or vice versa). But these conditions don’t wait their turn. They interact and reinforce each other constantly. Trying to treat them separately is like trying to put out a fire while someone keeps pouring gasoline on it.
This is why so many people with co-occurring disorders end up in what feels like a revolving door, cycling through different treatments, experiencing temporary improvements, then relapsing and ending up back where they started. It’s not that treatment doesn’t work. It’s that you’ve been receiving the wrong type of treatment.
What Integrated Dual Diagnosis Treatment Looks Like
Integrated treatment means your mental health and substance use disorder are addressed simultaneously by a coordinated team of professionals who understand how these conditions interact.
Here’s what truly integrated dual diagnosis treatment includes:
Comprehensive assessment of both conditions. From day one, clinicians evaluate not just your substance use history, but your mental health symptoms, trauma history, medical needs, and life circumstances. This complete picture guides your personalized care plan.
A unified treatment team. Instead of seeing separate providers for addiction and mental health, you work with an integrated team that might include a psychiatrist, addiction specialist, licensed therapists, and medical staff, all communicating with each other and working toward the same goals for your recovery.
Evidence-based therapies that address both conditions. Treatments like Cognitive Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT) are effective for both substance use disorders and mental health conditions. These therapies help you identify thought patterns that contribute to both depression and substance use, develop healthier coping skills, manage difficult emotions without turning to substances, and build a life worth staying sober for.
Medication management for mental health and addiction. For many people, medication is an essential part of dual diagnosis treatment. This might include antidepressants or anti-anxiety medications for mental health conditions, medication-assisted treatment (MAT) for opioid or alcohol dependence, or mood stabilizers for bipolar disorder. Psychiatric oversight ensures medications work together safely and effectively.
Personalized care plans tailored to your unique situation. There’s no one-size-fits-all approach to dual diagnosis. Your treatment plan should reflect your specific diagnoses, your life circumstances (work, other responsibilities), your treatment goals, and what’s worked or hasn’t worked for you in the past.
Family education and support. Addiction and mental health disorders affect your entire support system. Quality dual diagnosis programs include family education to help loved ones understand both conditions, improve communication, and build a support network that strengthens your recovery.
At Heartfelt Recovery Centers, this integrated approach is what we do. As Joint Commission accredited specialists in dual diagnosis treatment, we bring together psychiatric services, addiction expertise, and evidence-based therapies in personalized programs designed around your needs, not a standardized protocol.
Our Intensive Outpatient Program (IOP) and Partial Hospitalization Program (PHP) offer the flexibility to maintain work and other responsibilities while receiving comprehensive care for both your mental health and substance use.
Ready to experience integrated treatment? Contact Heartfelt Recovery Centers at (603) 207-1633 for a confidential assessment.

Evidence-Based Therapies for Dual Diagnosis Treatment
When you’re dealing with co-occurring disorders, the treatment approaches that work best are those with strong research backing, therapies that have been proven effective for both mental health conditions and substance use disorders.
Cognitive Behavioral Therapy (CBT)
CBT is one of the most widely studied and effective treatments for dual diagnosis. This therapy is based on the understanding that your thoughts, feelings, and behaviors are all connected. When you change unhelpful thought patterns, you can change how you feel and what you do.
In dual diagnosis treatment, CBT helps you identify thoughts that contribute to both depression and substance use (like “I’m worthless” or “I can’t cope without using”), challenge and reframe those thoughts, develop healthier responses to triggers and cravings, and build problem-solving skills for managing life challenges without substances.
CBT is practical and skills-focused, which means you leave each session with tools you can use right away.
Dialectical Behavior Therapy (DBT)
DBT was originally developed for people with borderline personality disorder but has proven incredibly effective for anyone struggling with intense emotions, impulsive behaviors, and difficulty tolerating distress (all common experiences for people with co-occurring disorders).
DBT teaches four core skill sets: mindfulness (staying present and aware rather than escaping into substances), distress tolerance (getting through difficult moments without making things worse), emotion regulation (managing intense feelings in healthy ways), and interpersonal effectiveness (communicating needs and setting boundaries in relationships).
For people with dual diagnoses, DBT is especially powerful because it addresses the emotional dysregulation underlying both substance use and many mental health conditions.
Trauma Therapy (EMDR)
If trauma is part of your story (whether it’s childhood abuse, combat exposure, assault, or other traumatic experiences), trauma-focused therapy is essential for lasting recovery.
Eye Movement Desensitization and Reprocessing (EMDR) is an evidence-based approach that helps your brain process traumatic memories so they no longer have the same emotional power over you. When trauma is properly processed, symptoms of PTSD diminish, and the need to use substances to numb trauma-related pain decreases.
Our trauma-informed care at Heartfelt Recovery Centers means we understand that substance use often developed as a survival mechanism in response to trauma. We work with you at a pace that feels safe, never pushing you to confront traumatic material before you’re ready.
Medication-Assisted Treatment (MAT)
For certain types of addiction (particularly opioid and alcohol use disorders), medications can be a critical part of treatment. Medication-assisted treatment (MAT) combines FDA-approved medications with counseling and behavioral therapies.
For opioid use disorder, medications like buprenorphine (Suboxone) or naltrexone reduce cravings and withdrawal symptoms, allowing you to focus on therapy and rebuilding your life rather than being consumed by the physical need for opioids.
For alcohol use disorder, medications like naltrexone or acamprosate can reduce cravings and make it easier to maintain abstinence.
When you also have a mental health condition, psychiatric medications like antidepressants, anti-anxiety medications, or mood stabilizers can be prescribed alongside MAT. Having a psychiatrist and medical team who understand how to safely combine these medications is crucial, and that’s exactly what you get with integrated dual diagnosis care.
At Heartfelt Recovery Centers, medication-assisted treatment is available as part of our comprehensive approach, always combined with therapy and personalized support to address all aspects of your recovery.
Recognizing the Signs of Co-Occurring Mental Health and Addiction
Sometimes it’s hard to know if what you’re experiencing qualifies as a dual diagnosis. Here are signs that you may be dealing with co-occurring disorders:
- You use substances to manage emotions or symptoms. If you drink when you feel anxious, use drugs to cope with depression, or rely on substances to sleep or face social situations, that’s a red flag.
- Your mental health symptoms worsen when your substance use increases. Pay attention to whether your depression gets deeper, your anxiety becomes more intense, or your mood swings become more extreme when you’re using more frequently.
- Previous treatment for either condition didn’t provide lasting results. If you’ve been to therapy for mental health but still struggle, or you’ve tried to quit using substances but can’t stay sober, co-occurring disorders might be the missing piece.
- You have difficulty managing daily responsibilities. Both addiction and mental health disorders can make it hard to maintain work, relationships, self-care, and other aspects of daily life. When both are present, these challenges multiply.
- Your relationships are suffering. Loved ones may have expressed concern about both your substance use and your mood, behavior, or emotional state.
- You feel hopeless about getting better. This feeling often comes from trying to address one problem while the other remains untreated. Integrated care can break through that hopelessness.
If several of these signs sound familiar, you’re not alone, and more importantly, help is available. Reaching out for a professional assessment is the first step toward understanding what you’re dealing with and getting the right kind of treatment.
Call Heartfelt Recovery Centers today at (603) 207-1633 for a confidential, compassionate assessment. Your privacy is our priority, and our dual diagnosis specialists are here to help.
Finding Hope Through Integrated Dual Diagnosis Treatment
Living with co-occurring mental health and substance use disorders can feel overwhelming and isolating. You might feel like you’ve tried everything, or like nothing will ever work. But here’s the truth: when you receive integrated treatment that addresses both conditions together, recovery is absolutely possible.
You’re not facing two separate problems. You’re facing one interconnected challenge, and that challenge requires one comprehensive, coordinated solution. Integrated dual diagnosis treatment brings together the medical care, psychiatric support, evidence-based therapy, and personalized attention you need to heal.
At Heartfelt Recovery Centers in Hudson, NH, we understand that your journey is unique. That’s why we create personalized care plans tailored to your specific diagnoses, your life circumstances, and your goals for recovery. Our Joint Commission accredited facility offers:
- Dual diagnosis specialists with expertise in co-occurring disorders
- Flexible scheduling with Intensive Outpatient (IOP) and Partial Hospitalization (PHP) programs that fit your life
- Evidence-based therapies including CBT, DBT, and trauma therapy
- Medication-assisted treatment and psychiatric services
- Family education and support to help your loved ones understand and support your recovery
- Personalized care that treats you as an individual, not a diagnosis
This Mental Health Awareness Month, take the step you’ve been considering. Whether you’re reaching out for yourself or for someone you love, know that compassionate, expert help is available.
Contact Heartfelt Recovery Centers:
📞 Call us at (603) 207-1633 for a confidential assessment
📍 Location: 41 Sagamore Park Road, Hudson, NH 03051
🌐 Learn more: heartfeltrecoverycenters.com
Your recovery journey starts with understanding what you’re really facing and finding the integrated care that addresses all of it. We’re here to walk that journey with you.
Heal. Grow. Thrive.
Frequently Asked Questions About Dual Diagnosis Treatment
What is the difference between dual diagnosis and co-occurring disorders?
Dual diagnosis and co-occurring disorders are two terms for the same thing: when someone experiences both a mental health condition and a substance use disorder at the same time. Both terms describe the need for integrated treatment that addresses both conditions together rather than separately.
Can you treat mental health and addiction at the same time?
Yes, and research shows this is the most effective approach. Integrated dual diagnosis treatment addresses both conditions simultaneously because they influence each other. Treating one without addressing the other often leads to relapse and incomplete recovery.
How long does dual diagnosis treatment take?
Treatment length varies based on individual needs, severity of conditions, and progress in recovery. Some people benefit from several weeks of intensive treatment, while others need several months. Treatment is personalized and adjusted based on your progress and goals.
Will my insurance cover dual diagnosis treatment?
Most major insurance plans cover dual diagnosis treatment. Heartfelt Recovery Centers works with most insurance providers and can verify your coverage at no cost. Our admissions team will help you understand your benefits before you begin treatment.
What happens during a dual diagnosis assessment?
A comprehensive assessment evaluates your mental health symptoms, substance use history, medical needs, trauma history, and life circumstances. This typically includes interviews with clinical staff, questionnaires, and sometimes physical health evaluations. The assessment helps create your personalized treatment plan.
Can I get dual diagnosis treatment while working?
Yes. Many people maintain their jobs while in treatment through flexible outpatient programs. Heartfelt Recovery Centers offers Intensive Outpatient (IOP) and Outpatient (OP) programs with evening and weekend options designed to fit work schedules.
What if I don’t know which came first, my mental health issues or my addiction?
It doesn’t matter which came first. What matters is that both conditions are affecting your life now and both need treatment. Integrated dual diagnosis care addresses both simultaneously regardless of which developed first.
Is medication always necessary for dual diagnosis treatment?
Not always. Some people benefit from medication for mental health conditions, addiction, or both, while others respond well to therapy alone. Medication decisions are made individually based on your specific needs, diagnoses, and preferences in consultation with psychiatric professionals.
Will my family be involved in my dual diagnosis treatment?
Family involvement is beneficial and encouraged, but not required. Many dual diagnosis programs offer family education sessions to help loved ones understand both conditions and how to provide support. The level of family involvement is based on your preferences and situation.
What makes Heartfelt Recovery Centers different for dual diagnosis treatment?
Heartfelt Recovery Centers specializes in integrated dual diagnosis care with Joint Commission accreditation. Our coordinated team of addiction specialists, therapists, and psychiatric professionals work together to create personalized treatment plans. We offer flexible outpatient programs that allow you to maintain work and responsibilities while receiving comprehensive care.
How do I know if outpatient treatment is right for my dual diagnosis?
Outpatient treatment works well for people who have a stable living environment, don’t need 24/7 medical supervision, and can commit to regular treatment sessions. During your assessment, clinical staff will recommend the appropriate level of care (PHP, IOP, or OP) based on your needs.
Can dual diagnosis treatment help with trauma?
Yes. Many people with dual diagnosis have experienced trauma. Trauma-informed care is integrated into dual diagnosis treatment, using approaches like EMDR and trauma-focused CBT to help process traumatic experiences safely while addressing both mental health and substance use.
What happens after I complete dual diagnosis treatment?
Recovery is ongoing. After completing initial treatment, you transition to continuing care which may include step-down levels of outpatient treatment, ongoing individual therapy, support groups, and regular check-ins. Aftercare planning ensures you have support systems in place for long-term recovery.
Heartfelt Recovery Centers is a Joint Commission accredited outpatient addiction treatment facility specializing in personalized, evidence-based care for substance use disorders and co-occurring mental health conditions. Serving Hudson, Nashua, Manchester, and southern New Hampshire and Massachusetts, we offer flexible Intensive Outpatient (IOP) and Partial Hospitalization (PHP) programs designed to fit your life.
Related Resources
- Learn more about our Dual Diagnosis Treatment program
- Explore our Intensive Outpatient Program (IOP)
- Discover our Partial Hospitalization Program (PHP)
- Read about Medication-Assisted Treatment options
- Learn about our therapy services
- Find out about our Suboxone Treatment program
- Verify your insurance coverage
References:
- Substance Abuse and Mental Health Services Administration (SAMHSA). “2019 National Survey on Drug Use and Health.” SAMHSA.gov.
- National Institute on Drug Abuse (NIDA). “Common Comorbidities with Substance Use Disorders Research Report.” NIDA.nih.gov.
- National Alliance on Mental Illness (NAMI). “Dual Diagnosis.” NAMI.org.
- Journal of Substance Abuse Treatment. “Integrated Treatment for Co-Occurring Disorders: A Review of the Evidence.” PubMed.gov.

MD Mitchell Grant Cohen
Dr. Mitchell G. Cohen is a board-certified Internal Medicine specialist with over 34 years of experience in patient-centered healthcare. A graduate of Hahnemann University School of Medicine, Dr. Cohen completed his internship at the University Health Center of Pittsburgh, where he gained invaluable hands-on experience. He is also a certified addiction specialist, holding membership with the American Society of Addiction Medicine (ASAM).
Currently based in Nashua, NH, Dr. Cohen is affiliated with Saint Joseph Hospital, where he provides comprehensive care focusing on both internal medicine and addiction treatment. His expertise includes prevention, diagnosis, and management of adult diseases, as well as specialized care for individuals facing substance use disorders.
Dr. Cohen is committed to fostering open communication, ensuring his patients are fully informed and empowered to make confident decisions about their health and treatment options.
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen
- MD Mitchell Grant Cohen







